Now let’s go over how your gynecologist will evaluate the bleeding. This will vary from doctor to doctor. However, the following three steps need to be done:
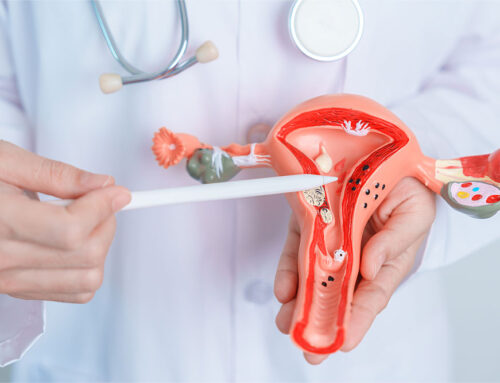
1. Pelvic exam – your doctor examines you thoroughly and look for any abnormality of the labia, vagina, cervix, rectum (for example hemorrhoids) and any pelvic masses. This allows your doctor to identify any source of bleeding other than the uterus. A papsmear should be taken if you are due for one (or it could be scheduled on a separate visit). A rectal exam could also be done if there’s no evidence of vaginal bleeding. However digital rectal exams are not sensitive enough and you might need a colonoscopy (Screening colonoscopy should be done at the age of 50 and in some cases at the age of 45).
2. Imaging with pelvic transvaginal ultrasound is done to look for pelvic masses and to measure the thickness of the endometrial lining (that is the inner lining of the uterus).
If the endometrial lining is thick and measures more than 4mm, then you should undergo evaluation of the endometrium.
If there is any fluid within the cavity of the uterus, I recommend evaluation as well.
If the endometrial lining is less than 4mm, I still offer optional evaluation of the endometrial cavity or close observation and repeating the pelvic transvaginal ultrasound within 3 months.
Another approach is sonohysterogram (also known as Saline Infusion Sonography SIS). This is a pelvic ultrasound done while injecting fluid inside the uterine cavity and allows your doctor to accurately evaluate the endometrial cavity and the endometrial thickness. It can also confirm the presence of polyps. SIS is much more accurate than transvaginal ultrasound alone.
It is important to know that ultrasound measurements are an estimation and that endometrial pathology could still be missed. So if the bleeding persists or recurs, I would recommend further evaluation even if the endometrial lining is less than 4mm.
Note: CT scan and MRI are not as useful as a pelvic transvaginal ultrasound or SIS to evaluate the endometrial lining.
3. Endometrial sampling is the most important step:
- to rule out any cancer or hyperplasia
- to find out if you have polyps and remove them
- and to can confirm atrophy
There are 2 ways to evaluate the endometrium:
- Office hysteroscopy with biopsy or curettage (which I recommend)
- Endometrial biopsy
Office hysteroscopy is much more accurate than endometrial biopsy. If your doctor offers office hysteroscopy then I would recommend that approach.